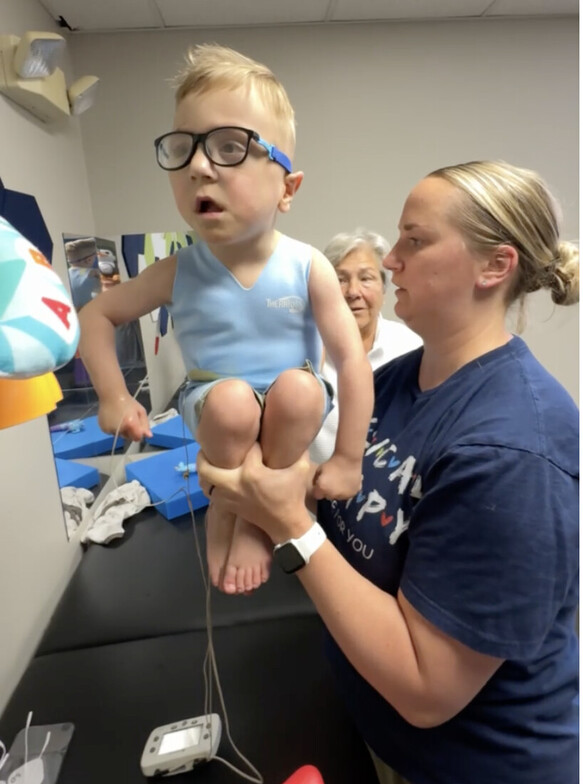
Dynamic Movement Intervention (DMI) is a relatively new pediatric therapy approach based on the principles of neuroplasticity—the brain’s ability to reorganize and form new neural connections.
DMI focuses on practicing very specific movements at a high level of intensity and repetition. This repetition is important because repeated movement helps strengthen neural pathways within the central nervous system, allowing children to develop new motor skills and improve control of their bodies.
DMI is also a highly structured and certified therapy modality. Each certification level requires 16 hours of live instruction, and therapists must wait a designated period of time between levels before advancing. This allows clinicians time to apply what they’ve learned in real-world settings and deepen their understanding before progressing. If you are seeking DMI therapy please ensure that your therapist has been properly trained.
Research consistently shows that neuroplasticity is most active in early childhood, particularly during the first five years of life. Because DMI relies on these principles, the approach may be especially effective during this developmental window. That said, children older than five can still benefit from DMI and any therapy that targets neuroplasticity and motor learning.
What Does the Research Say?
In the physical therapy world right now, there is a lot of discussion about evidence-based practice—and some debate about whether DMI meets that standard.
I fully support evidence-based practice and consider myself an evidence-based therapist. According to the National Institutes of Health, evidence-based practice typically involves the integration of three key components:
1. Best Available Research
This includes high-quality peer-reviewed research such as randomized controlled trials, systematic reviews, and meta-analyses.
2. Clinical Expertise
This refers to the clinician’s professional experience, training, and clinical judgment developed through years of practice.
3. Patient Values and Circumstances
This includes the goals, preferences, cultural considerations, and individual circumstances of the patient and their family.
When these three components come together, clinicians can provide care that is both scientifically informed and individualized. This approach helps avoid the “cookie-cutter” model of therapy, recognizing that two children with the same diagnosis may present very differently and require different treatment strategies.
Where Does DMI Fit Into This?
One of the strengths of DMI is that it is far from a one-size-fits-all approach.
Each level of certification includes 30–40 different exercises, and a typical one-hour DMI session may include 8–10 different activities. Therapists select exercises based on the child’s abilities, goals, and responses during the session, meaning each treatment plan is highly individualized.
Why Some Debate Exists
DMI has been around for roughly nine years, growing from just two founding therapists to thousands of trained clinicians worldwide.
High-quality research—especially randomized controlled trials—takes time to design, conduct, and publish along with securing large amounts of funding. DMI originated in clinical practice rather than in a research laboratory, meaning the approach was developed through therapists working directly with children and families.
There are currently clinicians and research groups working to collect outcome data with the goal of publishing more formal research in the future.
The Role of Clinical Experience
Clinical expertise is the second component of evidence-based practice.
I have been a physical therapist for nearly 13 years, the vast majority of which have been spent working in pediatrics. Over that time I’ve worked with many children and families, and I continue to learn and grow as a clinician.
While I would never claim to be the expert on any single therapy approach, I would also never continue using a technique if I did not see meaningful results for my patients.
Through my experience, I have seen children reach milestones that were previously very difficult for them—such as:
- Getting from the floor up to sitting independently
- Transition from walking with a walker to walking independently without a device
- Developing better head and trunk control so they can sit unsupported
- Taking their first independent steps
- Improving balance and functional mobility so they can participate with friends at recess
For many children, DMI has been a powerful tool that helped support progress toward these goals.
Families and Individual Goals
The third component of evidence-based practice—patient values and circumstances—is just as important.
Parents of children with disabilities are some of the most dedicated and determined individuals I know. They work tirelessly to support their children’s growth and development.
When families learn that early childhood is a critical window for neuroplasticity, many understandably want to explore therapies that may help their child make progress during that time. They don’t have the luxury of time to wait for the ‘gold standard’ research articles.
In addition to emerging research, we have case studies, clinical outcomes, and countless real-world examples of children gaining new skills through DMI-based interventions.
An Important Perspective
It’s important to emphasize that DMI is not the only modality I use in therapy. DMI has been a wonderful addition to my practice. As my favorite professor in PT school would say “it’s a great tool to put in my toolbox.”
Pediatric therapy includes many approaches, and while every child is unique, their therapy should reflect that. Some children may benefit from an intensive DMI program, while others thrive in play-based therapy sessions and others need referrals to other therapists or medical specialists.
So I will pose the question again, is DMI evidence-based?
At the end of the day, my goal as your PT is simple: To improve the quality of life of your child and your family.
With love and optimism,
Whitney
Resources:
- https://dmitherapy.com/
- https://www.nih.gov/
- Roos R. Current state of evidence-based practice in clinical physiotherapy. S Afr J Physiother. 2025 May 29;81(1):2139. doi: 10.4102/sajp.v81i1.2139. PMID: 40470171; PMCID: PMC12135705.
- Sackett DL. Evidence-based medicine. Semin Perinatol. 1997 Feb;21(1):3-5. doi: 10.1016/s0146-0005(97)80013-4. PMID: 9190027.

Whitney Williams
Contact Me